
Crypto Investment Entry and Exit Strategies of Institutional Investors
Section: Business
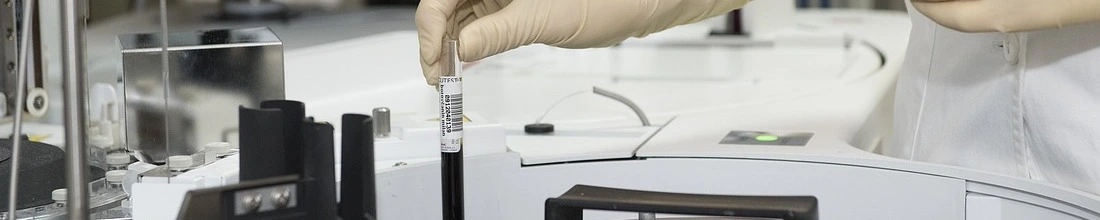
Cancer cells can escape from tumors, sneak through the bloodstream, and seed new tumors, or metastases, in distant organs. In a recent study of breast cancer, researchers captured the rogue individuals among these circulating tumor cells (CTCs) that metastasized to the brain - a deadly kind of metastasis. They hope to use these cells to understand the fundamentals of brain metastasis, and eventually to detect the early stages of metastasis and prevent it.
Almost all cancer deaths are caused not by the patient's primary tumor but by metastasis, and a sizable portion of breast cancers metastasize to the brain, explains Dr. Dario Marchetti, director of the CTC Core Facility at Baylor College of Medicine in Houston, USA, and senior author of the new Science Translational Medicine study. "We have a lot of drugs that can successfully treat primary breast tumors, but we do not have drugs that can effectively stop or treat brain metastasis."
"It's a fundamental problem because the brain appears to be a privileged site for a lot of therapies," says Dr. Luis Alberto Diaz, an oncologist at Johns Hopkins Sidney Kimmel Comprehensive Cancer Center in Baltimore, USA, who was not involved in the study. "Cells that survive in the brain have two advantages over other cells. One is the blood brain barrier that does not allow drugs into the brain. The second is that the cells are selected to migrate to, invade and thrive in the central nervous system."
There is growing interest in using CTCs to track the behavior of a tumor without repeated surgical biopsies. These non-invasive "liquid biopsies" could indicate if a patient's tumor is developing resistance to a drug, or if it has acquired different genetic mutations, which would require a change of drugs.
For reasons scientists still do not understand, only some CTCs from a patient's tumor can cause metastasis. Many of them probably die in the unfamiliar environment of the bloodstream, or cannot spawn a new tumor when they do settle in a new organ. Dr. Marchetti's goal was to filter out the tiny sub-population of breast cancer CTCs that can set up shop in the brain. Most likely, Dr. Diaz explains, the cells that cause brain metastasis have different physical and genetic characteristics than the bulk of the tumor cells.
Dr. Marchetti's research team sought to determine those characteristics by studying the circulating breast cancer cells. In collaboration with neuro-oncologist Dr. Morris Groves at the University of Texas MD Anderson Cancer Center in Houston, USA, Dr. Marchetti analyzed the CTCs from blood samples from 38 breast cancer patients. He was looking for a set of characteristics - markers for cell surface proteins - that previous research from numerous labs had implicated in metastasis.
The researchers found such a signature in a portion of CTCs from three of the patients. Those cells had a combination of four biomarkers. Two of them, Human epidermal growth factor receptor 2 (HER2+) and epidermal growth factor receptor (EGFR), are proteins that encourage cell proliferation and are linked to high risk of breast cancer brain metastasis. The third, heparanase (HPSE), is an enzyme that degrades the matrix surrounding tumor cells and allows them to break free and enter the bloodstream and then invade new tissue. The forth, Notch1, is a marker of stem cells and "tumor-initiating cells" that can cause metastasis.
Dr. Marchetti and colleagues grew CTCs with those combined four markers in culture to study their behavior and cancerous properties. Then they injected individual cells from these cultures into mice. The mice were bred to have virtually no immune system so they would not reject the human-derived cancer cells, which could then initiate new tumors in the mice. Those selected CTCs established new tumors in the mice, and a large majority of those tumors metastasized to the brain, compared to a small minority of the same patients' CTCs without that telltale brain metastatic signature. There is still much work to do, says Dr. Marchetti. His team is currently searching for other potentially important markers for metastasis or invasiveness.
Although this study may not yet have clinical significance and involves just a handful of patients, "it does represent another step in our understanding of the metastatic process," says Dr. Daniel Hayes, clinical director of the breast oncology program at the University of Michigan Comprehensive Cancer Center in Cleveland, USA, and who is an expert in breast cancer and CTCs.
An important future step will be to find compounds that prevent brain metastasis in animal models of breast cancer by selectively targeting these putative brain metastatic CTCs - and then develop anti-metastatic drugs for patients. That is where Dr. Marchetti hopes this research will ultimately lead, to predict and prevent metastasis in cancer patients.

Section: Business

Section: Arts

Section: Arts

Section: Business

Section: Business

Section: Arts

Section: Health

Section: Arts

Section: News

Section: News
Health Insurance in Germany is compulsory and sometimes complicated, not to mention expensive. As an expat, you are required to navigate this landscape within weeks of arriving, so check our FAQ on PKV. For our guide on resources and access to agents who can give you a competitive quote, try our PKV Cost comparison tool.
Germany is famous for its medical expertise and extensive number of hospitals and clinics. See this comprehensive directory of hospitals and clinics across the country, complete with links to their websites, addresses, contact info, and specializations/services.
One of the most beautiful squares transforms into a summer stage every year for two days. The Gärtnerplatz Open-Air features a free music and cultural program across three stages, as well as street food from local vendors. On Saturday, the main stage at Gärtnerplatz offers something for everyone,...

No comments yet. Be the first to comment!